What is CF? How can one 'get' CF?
Cystic fibrosis (CF) is a genetic disorder that primarily affects the respiratory and digestive systems. It is caused by a mutation in a specific gene called the cystic fibrosis transmembrane conductance regulator (CFTR) gene. This gene controls the movement of salt and water in and out of the body's cells, and in people with CF, the CFTR gene is mutated, leading to a buildup of thick, sticky mucus in the affected organs. In the respiratory system, the mucus clogs the airways and traps bacteria, leading to chronic lung infections, inflammation, and damage to lung tissue. This can cause breathing difficulties, coughing, wheezing, and a decreased ability to exercise or perform daily activities. In the digestive system, the thick mucus can block the pancreas and prevent digestive enzymes from reaching the small intestine, leading to malnutrition, poor growth, and weight loss. It can also cause intestinal blockages, abdominal pain, and diarrhea. Although CF primarily affects the lungs, it may also ultimately affect other organs such as the pancreas, liver, and intestines. In a normal individual, mucus is a crucial component of the body's natural defense system. It lines the respiratory and digestive tracts, acting as a protective barrier against harmful particles and microorganisms. The mucus in the respiratory tract traps these particles and microorganisms, and cilia (tiny hair-like structures) move the mucus out of the airways and into the throat, where it can be coughed up and expelled from the body.
In individuals with CF, however, the mucus becomes thick and sticky. In CF, the CFTR protein is either missing or not working correctly, resulting in the production of thick, sticky mucus. This gene provides instructions for making a protein that regulates the movement of salt and water in and out of cells in the body. The thick mucus in CF clogs the airways, making it difficult to breathe and increasing the risk of lung infections. It also affects the digestive system, blocking the ducts that carry digestive enzymes from the pancreas to the small intestine, leading to malabsorption and malnutrition.
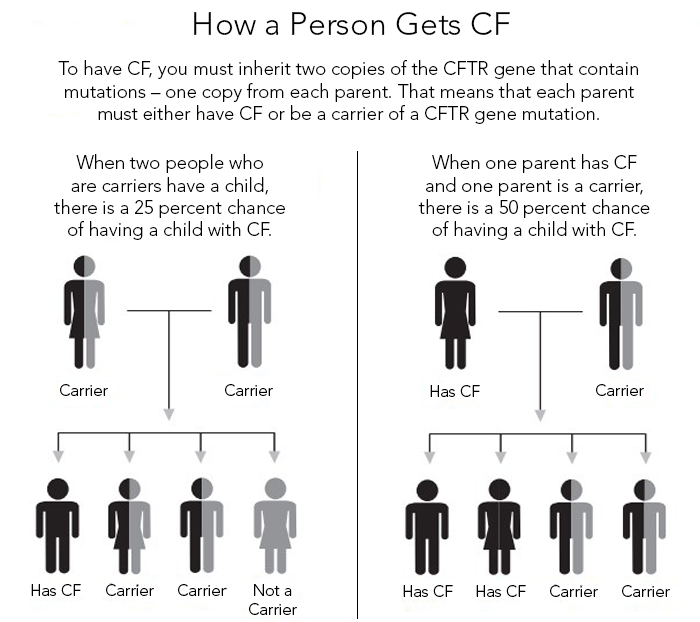
CF is a recessive genetic disorder, meaning a person must inherit two copies of the mutated gene (one from each parent) to develop the condition. If both parents are carriers of the CFTR mutation, there is a 25% chance that each of their children will inherit two copies of the mutated gene and develop CF. Approximately 1 in 35 Americans carry the CF gene, and CF is considered to be a rare disease.
What are the symptoms and what does living with CF look like?
Cystic fibrosis is a complex disease with varying symptoms, and the severity of these symptoms varies from person to person. In fact, even in the same individual, symptoms can improve or worsen over time. For some people, symptoms may not appear until later in life, often during teenage years or adulthood. However, those who are diagnosed with cystic fibrosis in adulthood typically have a milder form of the disease. However, the severity of the disease is also very much dependent on how early a person is diagnosed and how many lung infections occur throughout their life.
Individuals with cystic fibrosis have an elevated level of salt in their sweat, and parents often notice a salty taste when kissing their children. In addition to this, the majority of cystic fibrosis symptoms affect the respiratory and digestive systems.
Respiratory symptoms may include a persistent cough that produces thick mucus, wheezing, exercise intolerance, repeated lung infections, inflamed nasal passages or a stuffy nose, and recurrent sinusitis. People with CF have an extremely sensitive digestive system, and symptoms may include foul-smelling and greasy stools, poor weight gain and growth, intestinal blockage in newborns, and chronic or severe constipation that could eventually cause part of the rectum to protrude outside the anus (rectal prolapse). This is simply naming a few, and other diseases (such as diabetics) may also develop over time.
As a result of these factors, people with CF are particularly vulnerable to infections caused by specific bacteria, including Pseudomonas aeruginosa, Burkholderia cepacia complex, and Staphylococcus aureus. These bacteria can cause severe lung infections and are often resistant to antibiotics, making them difficult to treat.
How is CF treated?
Living with CF can be challenging as the disease demands daily treatments including lung and airway clearing therapies, nebulizations, and regular hospitalizations for IV antibiotics. In addition to taking daily medication, individuals with CF must consume digestive enzymes with every meal. While most symptoms are treatable, the disease is time-consuming and may worsen with age due to permanent lung damage.
There is currently no cure for CF, but treatment aims to manage symptoms and improve quality of life. This can include:
- Chest physiotherapy, which involves breathing exercises and physical therapy to help clear mucus from the lungs
- Medications such as bronchodilators, antibiotics, and anti-inflammatory drugs to manage lung infections and inflammation
- Pancreatic enzyme supplements to aid digestion and help the body absorb nutrients
- Nutritional counseling to ensure adequate calorie and nutrient intake
- Lung transplant in severe cases
Handling CF involves ongoing management and monitoring to prevent complications and optimize overall health. This may include regular doctor visits, medication management, regular exercise, and avoiding exposure to infections and environmental pollutants. It is also important for people with CF to stay up-to-date on vaccinations and participate in clinical trials and research studies to help advance treatment options.
What about this new 'miracle' drug, called Trikafta?
Trikafta is a medication used to treat cystic fibrosis (CF) in people who have a specific genetic mutation called the F508del mutation. It was approved by the US Food and Drug Administration (FDA) in 2019 and is considered a revolutionary treatment for CF. Trikafta works by targeting the underlying cause of CF, which is a defective protein called cystic fibrosis transmembrane conductance regulator (CFTR).
Trikafta contains a combination of three drugs that help correct the function of the defective CFTR protein, allowing for better movement of salt and water in and out of cells. This helps to thin the mucus in the lungs, making it easier to clear and reducing the risk of lung infections. Trikafta has also been shown to improve lung function, reduce hospitalizations, and improve quality of life for people with CF.
Trikafta is considered a miracle drug because it has shown unprecedented results in clinical trials, with some patients experiencing significant improvement in lung function within days of starting the medication. It has also been shown to be effective in people with more advanced stages of CF who were previously thought to be untreatable and who may have required a lung transplant. Trikafta represents a major breakthrough in CF treatment, offering hope and a better quality of life for people with this debilitating disease